Effects of apamin and charybdotoxin on endothelium independent vasodilatation: implications in the study of EDHF Endothelial derived hyperpolarizing factor (EDHF), together with endothelial derived NO and prostacyclin represent the major endogenous vasodilator hormone pathways (Coleman et al, 2004). Since the chemical nature of EDHF is uncertain, many studies have relied on pharmacological tools. Often EDHF described as the endothelial dependent dilation which is resistant to a combination of drugs that inhibit NO synthase (usually L-NAME) and cyclo-oxygenase (usually indomethacin) but abolished by those that block large and small Ca2+-activated K+ channels (BKCa and S Ca; with charybdotoxin plus apamin respectively). This approach relies on each of these drugs being selective for endothelial dependent responses. In the current study we have taken a different approach to most and performed experiments where inhibitors were added to endothelium denuded vessels after dilators induced stable vasodilatation. Male Wistar rats (200 ± 15.4g) were killed by lethal exposure to CO2. Second order mesenteric arteries were mounted in isometric wire myographs and vasomotor responses recorded as described previously (Harrington and Mitchell, 2004). In some experiments vessels were contracted with EC80 concentration of U46619, dilation was then induced by the addition of 3x10-6M acetylcholine or 3x10 -6M SNP. When either L-NAME (10-4M) or charybdotoxin (10-7M) plus apamin (5x10-7M) were added after acetylcholine the vasodilatation was immediately and completely reversed (Figure A and B respectively). In other experiments, endothelium independent vasodilation induced by SNP, were also reversed by charybdotoxin plus apamin, but not L-NAME.
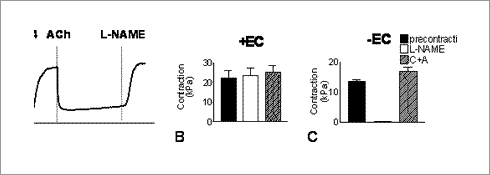
Figure A. Example trace of an artery re-contracting following the addition of L-NAME in pre-contracted arteries dilated with acetylcholine. Bar Graphs show re-contraction of arteries in response to L-NAME or charybdotoxin plus apamin (C+A) in arteries with endothelium, dilated with acetylcholine (Figure B) or without endothelium dilated with SNP (Figure C). This data demonstrates that charybdotoxin and apamin have pharmacological effects independent of the endothelium, at the level of smooth muscle cell function. These observations suggest results obtained with these drugs in relation to EDHF studies, should be treated with caution.
Harrington L and Mitchell JA (2004) Br J Pharmacol143: 611-617 |