Adverse Event Profiles of the Anti-Epileptic Drugs Lacosamide and Pregabalin, as Adjunctive and Mono-Treatments. Of adult epilepsy sufferers, 30%-50% do not take their medication correctly, (1), which can lead to an increase in morbidity and mortality (2). New antiepileptic drugs (AED) are administered adjunctively (3), and the adverse event (AE) profiles are a leading reason for poor adherence. Some newer AED, like lacosamide and pregabalin, are also licensed as mono-therapies in other conditions such as neuropathic pain (NP). A meta-analysis was performed to assess the AE profiles of lacosamide and pregabalin as adjunctive and mono-therapies. RCT were selected with adjunctive and mono therapy options. The adjunctive treatments were partial epilepsy RCTs and the mono-therapy NP RCTs, including diabetic neuropathy. Search criteria were partial epilepsy, adjunctive, lacosamide/pregabalin and NP. The RCTs were placebo controlled, double blind and participants aged >16 years. AE for treatment and placebo groups were extracted. Primary outcomes were total AE, and the three highest frequency AE for each drug respectively. Data bases used were PubMed, Science Direct, Springer Link and clinicaltrials.gov to August 2014. Quantitative analysis was by RevMan 5.2 (Copenhagen, Nordic Cochrane Centre, 2012). Fixed effect Mantel-Haenszel models were used to calculated Relative Risk (RR). Number needed to harm (NNH) and treat (NNT) were calculated and significance determined by Z statistic. Lacosamide produced 902 titles and screened to 339 abstracts for epilepsy and 238 for NP. 7 papers matched the criteria (3 for epilepsy, 4 for pain). For pregabalin the searches returned 5557 titles, screened to 622 for epilepsy and 1001 for NP, and 8 papers matched the criteria (4 for each). In a number of potentially viable trials, there was a lack of placebo data. A number of reports used duplicate data from 3 trials. Each trial has been included singly. Forest plots of 95% confidence intervals showed good statistical heterogeneity.
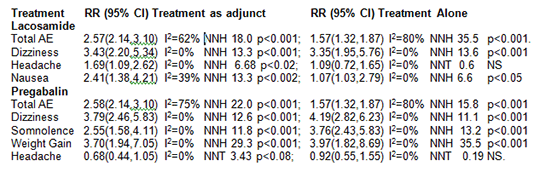
The incidence of AE for lacosamide adjunctive therapy increased two fold over when given alone, whereas pregabalin reduced by 30%, due to a trend towards improvement in headaches and no real changes in the other parameters. Of the three most common AE, lacosamine dizziness remained the same, but headache and nausea worsened. Pregabalin when given as adjunctive therapy is better tolerated than lacosamine. 1. Brown IP et al., (2009). Epilepsy Behav 16: 634-639. 2. Hodges JC et al., (2014). ISRN Pediatr 734689. 3. Ryvlin PE et al., (2008). Neuropsychiatr Dis Treat 4: 1211-1224.
|